CODA Craniocervical Dysfunction Initiative (CCD)
What is the CODA CCD Initiative?
The CODA Craniocervical Dysfunction (CCD) Initiative investigates how altered neuroimmune signaling at the craniocervical junction contributes to the initiation and progression of complex chronic disorders.
CODA’s initiative studies craniocervical dysfunction as a biologically anchored model system to better understand the mechanisms that drive complex multisystem illness.
What is Craniocervical Dysfunction?
Craniocervical dysfunction refers to abnormalities affecting the stability or alignment of the craniocervical junction. These disruptions can alter communication between the brain, spinal cord, and body-wide regulatory systems.
The craniocervical junction, where the skull meets the upper cervical spine, contains critical neural and vascular structures that regulate autonomic, immune, metabolic, and neurological functions. When biomechanical instability or structural compression occurs in this region, it may disrupt these systems and contribute to widespread symptoms across the body.
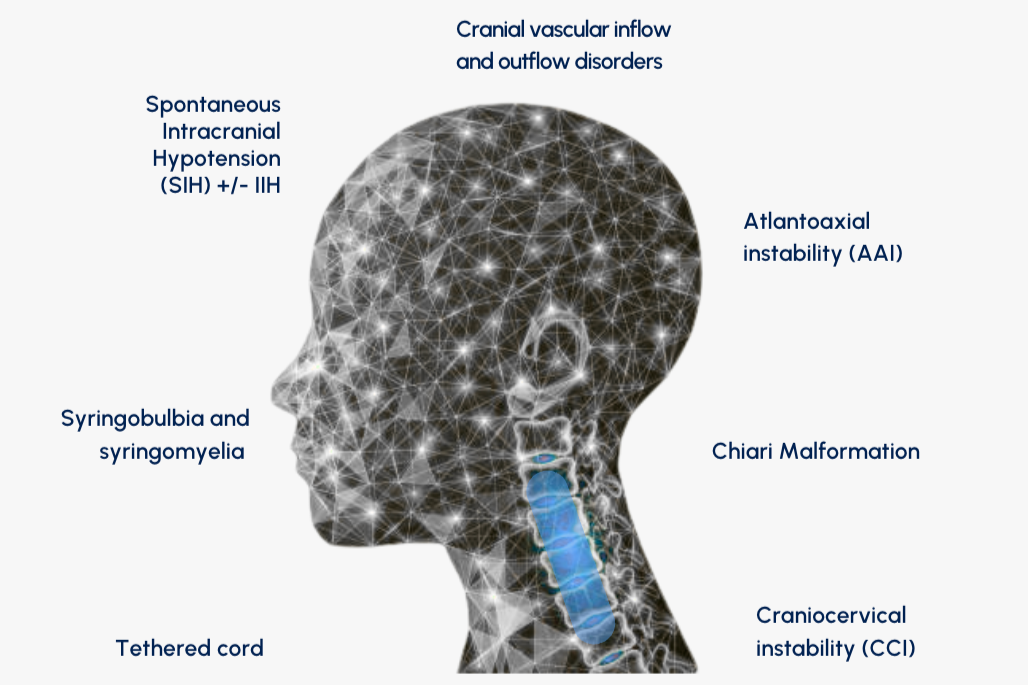
Clinically, patients may receive diagnoses related to craniocervical dysfunction including:
Craniocervical instability (CCI)
Atlantoaxial instability (AAI)
Chiari malformation
Syringobulbia and syringomyelia
Cranial vascular inflow and outflow disorders
Tethered cord
Spontaneous intracranial hypotension (SIH) with or without intracranial hypertension (IIH)
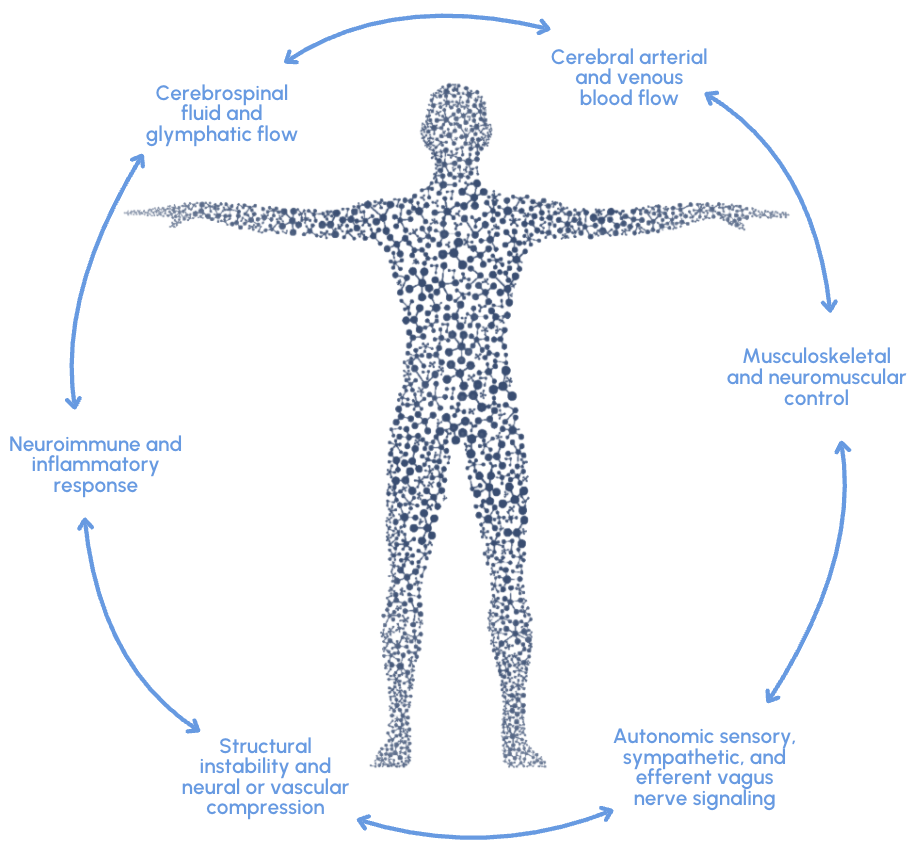
These structural changes may affect key physiological systems including:
Autonomic nervous system regulation
Neuroimmune signaling
Cerebrospinal fluid and glymphatic circulation
Cerebral arterial and venous blood flow
Sensory and vagal nerve signaling
Musculoskeletal and neuromuscular control of the head and neck
Why is CODA Studying Craniocervical Dysfunction?
Many individuals living with complex chronic illnesses experience severe symptoms despite limited findings on conventional diagnostic tests. This disconnect has slowed progress in identifying underlying mechanisms and effective treatments.
Craniocervical dysfunction provides a unique opportunity to study these conditions as a localized structural disruption at a critical neuroregulatory interface.
By examining how abnormalities at the craniocervical junction affect biological systems, researchers can explore how disruptions in this region contribute to broader multisystem dysfunction.
Rather than positioning it as the sole cause of complex disorders, CODA uses craniocervical dysfunction as a human model to investigate shared disease mechanisms. Anchoring multisystem symptoms to a defined structural issue allows researchers to study how disruptions at this junction influence neuroimmune, autonomic, and cognitive function.
Insights from this work may advance understanding of craniocervical dysfunction while revealing mechanisms relevant across multiple complex disorder
Steering Committee
-

Mikki Tal, PhD
Director, Center for Neurorestoration, Massachusetts Institute of Technology
-

Brayden Yellman, MD
Medical Director, Bateman Horne Center of Excellence
-

Ilene Ruhoy, MD, PhD
Director, Neuroimmune and Connective Tissue Neurology Program, Atria Health Institute
-

Mijail Serruya, MD, PhD
Director, Raphael Center for Neurorestoration. Thomas Jefferson University
-

Lauren Natbony, MD
CEO & Medical Director, Integrative Headache Medicine of New York
-

Peter Rowe, MD
Professor of Pediatrics, Johns Hopkins University
-

Nancy Klimas, MD
Director, Neuroimmune Medicine, Nova Southeastern University
-

Petra Klinge, MD, PhD
Professor of Neurosurgery, Brown University
